
June 20th, 2018 by Janine
A fire has started at the bottom of my ribs. It caught hold in an instant. Creeping upwards, slowly at first but I know what’s coming…it’s picking up pace…then whoosh; my chest, head, face and whole body is washed with heat. Fever type heat, taking over the lymph nodes, my forehead, my entire skin. All my sweat glands are working overtime and can’t compete, they give up. It’s a hot flush or flash and boy is it flashy. It makes its presence known.
Now, I’m hot and wet. Nup. Not that kind. The kind where you feel grubby, like you need a shower and a change of clothes. The night sweats are the worst (well for heat), waking up absolutely drenched, the bed linen soaked and feeling too hot to sleep (if I had any in the first place) …and knowing it will happen again in 10 minutes or an hour (if I’m lucky).
The worst is when you get up, feel good, have a shower, do your makeup, still feel good and then while you are finishing off drying your hair or just as you leave the house or need to head for a train…. whoosh it happens again…. that good feeling a distance memory when frustration, feeling stinky and in need of a second shower takes over. Decisions; go out sweaty or be late and have another shower. Lovely. Stinky wins most of the time. I hate being late. I feel like a woman of the Victorian age as I spray myself with perfume to cover up the body odour.
Mid-life crisis or Climacteric or ?
Speaking of ages and eras, I googled menopause and synonyms came up; maturity, mid-life crisis, climacteric, grand climacteric (no less), matureness, post maturity. Mid-life crisis – what an unhelpful way to talk about menopause. Though finally and slowly, Menopause is being talked about (mind you, we could do with a royal to take up the band wagon and bring it into the bright light). Climacteric is an interesting one, apart from referring to Menopause in medical circles it also denotes a critical period or event and having extreme and far-reaching implications or results. I got a shock when I discovered what some of these far-reaching implications were. Men, this is just one of the places where you come in!

Shock
In the week when I decided to research Menopause and Cancer the universe must have been aligning; three different sources of Menopause information happened into my path. The first one; I turned on the radio and heard the presenter say a piece on Menopause was coming up. Perfect timing.
Menopause; a completely natural process involving women’s bodies producing less oestrogen and changing progesterone hormone levels. I’ll come back to the implications of these in part two of this blog. For now, let me tell you about something I heard on the radio that shocked me. The host talked of how she had discovered some high flying, dynamic women at the top of their career had left their jobs due to the difficulty they had experienced in managing the symptoms of menopause.
Shocked doesn’t really explain it. In this day and age? I didn’t doubt that the symptoms must have been horrendous; I was stunned that women were not being adequately supported by medicine or natural means to enable a normal physiological transition to be facilitated so that their lives and work were not impacted in such a significant way. The feminist in me wondered if men would have put up with this state of affairs though to be reasonable, menopause appears to be a learning curve for many of us. Consequently, I was shocked.

I was even more shocked when men joined the discussion and explained their relationships had broken down, divorce had resulted and they described their many regrets about not having understood what the women in their lives were going through during menopause.
Job loss, love loss. OMG. Menopause, you can be incredibly cruel and we need to talk about you, a whole lot more. Now!
Symptoms and Years
In my humble opinion, Menopause symptoms are sh*t: mood swings, hot flushes, night sweats, brain fog, short term memory loss, difficulty in finding words and string sentences together, fatigue, low libido and vaginal dryness. They often start when women are in their 40s and 50s though can start when women are much younger.
Symptoms often last YEARS. Men, please note this. YEARS not weeks or months. Most women (8 out 101) face life impacting menopause symptoms for between 3 and 7 years and for some women, the rest of their lives. On top of this, perimenopause (the few years before menopause starts) usually brings unhelpful, generally unwanted symptoms too including disrupted sleep, headaches and heavy periods.

Ok, not all women experience these symptoms so we must be careful of making assumptions however MOST women do find themselves having to go through yet another massive learning curve about their body. And guys, it would be great if you came along for the educational ride. Not least because men go through a ‘pause’ of sorts too!
For men, it’s called andropause and refers to age-related changes in male hormone levels. Male menopause (not necessarily a helpful term) involves a drop in testosterone production in men who are age 50 or older. It’s often affiliated with hypogonadism. Both conditions involve lowered testosterone levels and similar symptoms.
You’re getting on my wick…
Ha. So we DO have an excuse for being irritable and bitchy. Sort of…well, not really…because it’s not that helpful, is it? Usually most of us just feel worse when we let irritation get the better of us and say or do something we wish we hadn’t said or done. However, when we know hormones may be playing a big part in our mood we can use our awareness to catch ourselves in our irritation and then choose our words and actions carefully, with more sensitivity. Not always easy but likely to result in a better day. It’s also OK to acknowledge we are feeling easily irritated!!
The more we talk about menopause, the more men and women will be able to identify when peri-menopause and menopause start. We can then learn about the options for managing the unhelpful symptoms. Finally, both men and women can then practice and take responsibility for being supportive, tolerant and understanding of each other and ourselves as we go through these changes. Maybe then, we’ll be able to avoid mountains from molehills and the extremes; relationship challenges and break down, negative outcomes for career and lifestyle.
Now imagine dealing with all of this…and cancer…and chemo.
Except, there’s more.
Identity
I wish it was just the symptoms listed above and the frequent embarrassment that accompanies them, that many women were dealing with. Going through the menopause can play havoc with women’s sense of identity, sexiness, and value in the world. Western society still predominantly relates to the menopause phase as women becoming old and somewhat invisible rather than being mature, loving and fully living life.
Edna M. Astbury-Ward summed it up well in her 2003 paper
The social construction of menopause as the entry point to old age may represent a challenging and difficult time, because while women may feel young, society tends to perceive them as rather less attractive and less fully functioning. This perception of menopause as a negative milestone is often found only in Western cultures. Medical culture also influences the meanings of middle and old age, particularly for women at the time of approaching menopause.
Cultural bias against ageing and sexuality has contributed to that stereotyping of older women as asexual. In general, the media has not served the ageing female well. Older men are often marketed as sexy, yet older women are rarely seen outside of advertisements for hormone replacement therapy (HRT) and Conti knickers.2
I suspect we need a new, positive and helpful narrative for the completely natural yet often difficult to go through transition that is menopause. The recent menopause cafe phenomenon may be helping with this as a space is provided to discuss menopause and challenge stereotypes.³ Princess Anne, Duchess of Cambridge, Kate; Duchess of Sussex, Meghan – you don’t fancy taking up the band wagon, do you?
Chemo vs Menopause
This was the backdrop to my realisation that chemotherapy and menopause symptoms are eerily very similar. I had been struggling to manage some of the chemo symptoms, particularly the lack of good quality sleep yet they may not have been chemo side effects at all (or at least not current side effects).
My next challenge along this cancer journey was now starkly obvious; to work out how best to support myself over the next year of treatment or to review treatment options, I needed to discern what was a chemo symptom and what was a menopause symptom and then learn how to address each in the best way for me. In the back of my mind it also occurred to me that I may end up going through this whole process twice so getting a handle on it was crucial to enjoying my life and living it to the full. Twice, because my menopause was possibly chemotherapy induced and not following its natural path. I was yet to find out if there was a chance my symptoms would stop then start again once chemotherapy was complete (joy of joys).
There it was, a whirlpool of thoughts swirling around, when in the space of a few days, I turned on the radio at the right time, walked into a foetal medicine building to use the loo only to discover a medical exhibition on menopause and noticed a webinar series advertised on social media involving a week of interviews where experts in menopause shared their pearls of wisdom.
Timing and attention; thank you, Universe.
Part two coming up -– the nuggets from the Menopause experts and my oncologists’ stand-off!
I am going to take a breather now… oh, and another shower.
References
1 https://www.nhs.uk/conditions/menopause/symptoms/
2 Astbury-Ward, E. (2003) ‘Menopause, sexuality and culture: Is there a universal experience? Sexual and Relationship Therapy’. Journal of the British Association for Sexual and Relationship Therapy. 18(4), 437-445
³ https://www.theguardian.com/society/menopause – Menopause café and challenging stereotypes about aging.
Acknowledgements
Images: Unsplash:
Steam_skyler-king-527288;
Shock_andre-guerra-676198;
Divorce_rawpixel-666933;
Sleep_vladislav-muslakov-261627
© 2018 Janine Hayward www.psychingoutcancer.com. All rights reserved.
Posted in Menopause, Myeloma Treatment, Symptoms and Side Effects Tagged with: Cancer, Chemotherapy, Menopause, Myeloma, Side effects, Treatment

I’d be pulling my hair out over the steroid incident (see last post) or I would be, if it wasn’t falling out, on its own accord. I’d be pulling my hair out over this week’s incident: a miscommunication between the Clinical Trial team and the Lab that makes up my chemo drugs resulting in me having to wait an extra three hours, until after 5pm, to be hooked up and receive my treatment. I didn’t get home until late and that meant less recovery and down time than I usually have on a Monday. Well, I would be pulling my hair out over this, if it wasn’t already receding at what seems like a rapid rate and coming perilously close to exposing my devil’s horn. I only have one (maybe I do things by halves after all!) bump of calcified bone formed from hitting my head a million times over my life time: on open cupboard doors, someone’s elbow when standing up, fridge doors, you name it I’ve managed to bump that same place on my head in some extraordinary ways! Hair loss and receding hairline, missed steroids and treatment delays. More, thank you Chemo, moments.
I know I’ve been lucky: I started with a lot of hair. A lot! Unlike many people going through Chemo for breast cancer and cancers other than Myeloma, my treatment is not usually linked with complete hair loss. I would not be a sexy bald (though have decided to do my best to embrace it, if it does happen). It is stressful to see the masses of hair come out in my fingers, in the sink, in my brush, in the air.

Hair loss – today’s right hand scoop – a light day (yay!)

Hair loss – today’s left hand scoop – a light day (yay!)

Hair loss – today’s offering
I’ve lost about a third of the volume so far. My hairdresser K, who I’ve known since 1993 (longer than my hubby and my ex!) knows my hair well and confirmed I wasn’t dreaming this. I am fortunate: I have regrowth already. Well lucky of sorts. The regrowth is crazy curly and goes out at right angles. Hubby nicknamed my curls, Turkey Twizzlers. Helpful. Giggle.
With my hair down, things are hidden and a bit tidier but the odd curl makes its way out over the day and spooks me when I look in the mirror – how long has it been jutting out like that ???!! OK curls can be cute (very very beautiful in fact, like those that adorn my sister-in-law and gorgeous niece) however a whole heap around my face when I am used to waves and straight hair takes some getting used to (as I imagine being bald does too). The curls are also resistant to smoothing serums and are frankly unmanageable. I give up. I hope they hurry up and grow long so gravity straightens them out.
Growing. Regrowth. That’s a good sign, isn’t it? The Chemo can’t be killing off all the good cells. Surely my nails and hair wouldn’t grow if my body didn’t tolerate the Chemo well, most of the time at least (and when I get my steroid on the right day, not bitter, can you tell?!). My nails, will I jinx them saying this? They seem super resilient so far… I hope it lasts. For the first time that I remember, my results show I’m calcium deficient so now I’m on an extra tablet for that and reintroducing halloumi and mozzarella.

New Curls
Sticky eyelids and thin skin
Hair loss, sticky eyelids, thin skin that leads to blisters or adhesive grazes when they wouldn’t normally occur are just some of the small and large niggles cancer and chemo have added to my life. Sticky eyelids are frustrating…I’m constantly pulling at my lashes to ‘release’ my eyelid from my eyeball. Refresher drops help a little though the stickiness quickly returns. Are there any advantages to sticky eyelids? I can’t think of any? Do let me know…
I put on a favourite super comfy pair of boots and invariably on a day when I’m running for a train or having to do loads of walking, five minutes in, I have a blister. Pre-chemo I wouldn’t have had a blister – its why I put these boots on after all! Scrabbling around for plasters, hoping they’ll stay on, too late, damage done, now nothing works. I revert to trainers as soon as possible.
Anyway, back to hair. What to do? Regain has been suggested. K has told me some of his clients also living with cancer have had great success with it though its best started as early as possible. What do you think – should I give it a go? I suspect it would possibly be introducing a toxin however is it a worthwhile trade-off? Every week there is something new that I think needs my attention and involves time consuming research yet if I don’t do it, I feel like I’m not doing the best I can do. It’s so exhausting.
Psychology
Body changes
Changes in body image will take getting used to and as always require kindness and compassion. It can be helpful to look in the mirror and look for what I love and am grateful for and not just focus on the unwanted changes.
For some people, hair loss is one of the most difficult aspects of living with cancer treatment as it can be entwined in their personal sense of self, preferred way of presenting self to the world and identity. It can also be tied up with ideas and assumptions about what it is to be feminine, masculine, young, virile, strong and attractive to others. Hair loss can trigger anxieties or trauma associated with earlier life experiences where people received unhelpful comments about the way they looked.
Society influences about what hair should be like overall, or at certain ages or what a hair style represents can also trigger unhelpful assumptions, rules and thoughts such as I must cover up my baldness, no one will find me attractive, I’m no longer feminine/masculine therefore there is no point being open to a new partner, friends won’t want to be seen with me so I shouldn’t meet up with them.
Hair loss and anxiety relating to hair disorders can be extremely distressing for some people…however you do not need to put up with it. Talking therapy with a psychologist can help with the distress. Therapy can help you uncover your thoughts and feelings about your hair and image, discover what is helpful and unhelpful, what is keeping distress going and identify new strategies to try out that nurture your identity, social interaction and self confidence. Therapy can help you accept your new or current image and not be stopped by any unhelpful thoughts about it.
Trichotillomania and Alopecia
There are many other difficulties relating to hair that people live well with live every day. Trichotillomania and Alopecia are just two of those. For those that experience great distress about these talking therapy can also help in similar ways as described above. If distressed, if one of these conditions is stopping you feeling like you or doing the things you want to do – don’t go it alone – a psychologist can help.
Trichotillomania (trik-o-til-o-MAY-nee-uh). Sometimes referred to as hair-pulling disorder, is a mental disorder that involves recurrent, irresistible urges to pull out hair from your scalp, eyebrows or other areas of your body, despite trying to stop.1
Alopecia and Alopecia areata. Alopecia refers to hair loss generally while alopecia areata refers to a specific, common cause of hair loss that can occur at any age. It usually causes small, coin-sized, round patches of baldness on the scalp, although hair elsewhere such as the beard, eyebrows, eyelashes, body and limbs can be affected. Occasionally it can involve the whole scalp (alopecia totalis) or even the entire body and scalp (alopecia universalis).2
Mental Health Awareness Week
By the way – It’s mental health awareness week in the UK and this year the focus is on stress. More about it here https://www.mentalhealth.org.uk/campaigns/mental-health-awareness-week. Talking about mental health helps to reduce stigma. I know I’ve said I don’t always welcome being asked ‘how are you?’ however that mostly related to diagnosis and early treatment days of living with cancer. I encourage you to tell someone how you are feeling. If you can ask someone else who you suspect may be feeling low or anxious or whose behaviour has changed (they’ve become more withdrawn, don’t seem to enjoy the things they used to enjoy or you notice appear to be struggling) if they want to talk. 5 minutes can make a huge difference. You don’t have to say anything special, just listen, acknowledge what they are saying and help them understand they are not the only ones to feel that way.
I know this because I work with people every week who share their experiences and symptoms. Research tells us1:
- Worldwide – Major depression is thought to be the second leading cause of disability worldwide and a major contributor to the burden of suicide and ischemic heart disease
- UK – Approximately 1 in 4 people in the UK will experience a mental health problem each year
- England, 1 in 6 people report experiencing a common mental health problem (such as anxiety and depression) in any given week.
- USA – Approximately 1 in 5 adults—43.8 million, or 18.5%—experiences mental illness in a given year.
- Australia – Almost half of the total population (45.5%) experienced a mental disorder at some point in their lifetime
- NZ – one in six New Zealand adults (16%, or an estimated 582,000 adults) had been diagnosed with a common mental disorder at some time in their lives.
Each person’s circumstances and road/process of recovery and managing mental ill health may be different yet there are often commonalities of impact on lives and symptoms.
Just imagine, this week might be the week you seek help or offer help to someone living with stress or living with the stress of cancer. What a difference you will make maybe without even knowing.
Then think of me with a Donald Trump style comb over. IT IS NOT GOING TO HAPPEN!
References
1 https://www.nhs.uk/conditions/trichotillomania/
2 http://www.britishskinfoundation.org.uk/SkinInformation/AtoZofSkindisease/AlopeciaAreata.aspx
3 see Mind and Mental Health Foundation and National Health Alliance on Mental Illness, Australian Government – Department of Health, NZ Mental Health Foundation for references and other details
Acknowledgements
Images: Upright Hair – mohamed-nohassi-531501-unsplash & Me
© 2018 Janine Hayward www.psychingoutcancer.com. All rights reserved.
Posted in Psychology for Cancer, Symptoms and Side Effects Tagged with: Alopecia, Alopecia areata, Cancer, Chemotherapy, Hair, Hair loss, Myeloma, Psychology, Receding hairline, Side effects, Sticky eyelids, Trichotillomania

April 18th, 2018 by Janine
Sick as a dog, thank you Chemo. I am meant to be on top form tomorrow. It’s hubby’s very special birthday and we have a full day of fun planned. Thanks, thanks a million for deciding to be ‘a bad Chemo’ day. Team, my wonderful team, I feel let down. There has been a mistake. You forgot to give me my steroids. I trusted you. I felt safe. I wasn’t safe today. It made a difference, a huge difference. I let myself down too. I forgot to do my own checks. I forgot to ask for my steroids. Consequences. There are always consequences in this Cancer game, some big, some small, some easily remedied, others drastic and most, a right pain in the arse. Consequences, you can rip the rug right out from under my plans. A plan to; feel good, not have to go near a hospital and not have to be in, manage my mood mode because something unexpected and unhelpful has triggered me.
Monday, you didn’t start out a bad day. In fact, you were brilliant until 6pm. I went for my morning blood test, at 8.30, later than usual after a wee welcomed sleep in and a fab, fun, friends packed day, on Sunday. Then, I moseyed to a café near hospital to do Italian language practice before my lesson with the fabulous C from Sardegna. I wandered back to Macmillan to a meeting with my therapist who helped me think about my recent test results, the meaning I was adding and my plans to up the ante on the work front. As usual she was a great help. My pink smoothie, a nutri-bulleted beetroot and green salad was yummy. My call with friend and coach M, was great. Even Chemo went smoothly. Or so I thought.
I got home and started feeling wretched. More wretched than I have in ages after a Chemo day. Even drinking water was difficult. Pain, everywhere. Nausea, constant. Stuck close to the bathroom. The Dom anti-nausea pill wasn’t doing its thing. Sweat, cold, sweat, cold. Aaargh. Why? Why today? This is sh*t. Will I function tomorrow? Hubby’s birthday is so important to me. He has even taken the day off work which is so rare. 10.15pm rolls around and Chemo you bit*h, you have me sitting on the couch, head in hands and between my knees.
Steroids

Then it dawns on me. I didn’t receive my steroids today. Dexamethasone, I wasn’t given it and I was so busy watching Americans on Prime to distract me from any pain of the cannula going in, that I didn’t do my own checks. Bugger. Now what. Now, I’ll have to telephone the Haematology Registrar on-call and see if I can take my day 16 (tomorrow’s dose) of Dex now. It’s not a great time of day to be taking a steroid, they’ll keep me up all night…but hopefully I’ll feel better. Priority right now: feel better.
Then I realise. Pissed off. If I take the dose I have at home, I’m going to have to go to hospital tomorrow now, the very day I didn’t want to go and normally don’t have to go near it. And on your birthday, darling Man. I don’t know how long it will take, to pick up a steroid on a day I am not usually there. VERY PISSED OFF. My feeling wretched, my having a problem, my having to go into problem solving mode, my having to deal with the impact, accept the consequences, pissed off…it was all so preventable. Annoyed. Sad.
I ring the hospital, ask for the Haematology Reg on call. Operator says she‘ll page him and he’ll call me back very soon, often straight away. I wait. 40 minutes later, I’m still waiting. I’m so sick, I can’t get angry. Hubby calls. The operator is surprised I haven’t heard. She pages him again. He calls back in 5 minutes. No apologies, no explanations (e.g on another call). He runs through the usual questions – have a vomited? Not yet. Do I have a temperature? No, just the sweat, cold combo. Do I have diarreah or constipation? No. Just pain, a lot of pain and nausea that pills don’t kick. Finally, he confirmed I should take the Dex I have at home and go up to hospital for another dose tomorrow.
I take the steroids and Hubby manages to find another stronger anti-nausea tablet amongst my large array of pills in ‘the pill box’ (a large bread bin, works a treat). I cuddle up to Hubby, focus on his breathing and wait for drugs to kick in. By the time we move it’s 1am and despite the steroid, I feel like my body is now desperate for sleep. Good. Happy to oblige. I drag myself upstairs to bed.

Hubby’s birthday day. I feel a whole heap better but very drained. He drives me to hospital. I go to get my steroid and my fear about how the day may unfold starts to be realised. Cancer, you bit*ch, you don’t make life easy. My steroid isn’t ready. I don’t get to drop in, collect it and get out again (my hope). Despite having an email back from my specialist in the morning, acknowledging that a) my Chemo, carfilzomib is hard to tolerate without the steroid and b) containing his request that I be dispensed the steroid today, directly from the Chemo Day Unit (CDU) and c) that the clinical trial nurse should call the CDU nurses to make sure they have the steroid ready for 9.30am – it’s not ready. I even get there about 10.40am, figuring I’d give everyone a bit more time to communicate and prepare.
I explain again, what has happened. The CDU nurses won’t give me the steroid and when they call the Clinical trial nurse for information something is lost in translation so they now think they need a prescription before they can give me anything. I show them my box of Dex with the prescription and dose details AGAIN. I start to get upset. Really upset. I could be waiting for ages for the clinical trial nurse to come to the CDU with a prescription (I’ve been through this before so know how long it can take) and then if I must go to the regular hospital pharmacy for it to be filled, I can write off another hour, it is hideously inefficient.
Tears. Yep they’re coming. I cry. M the wonderful receptionist comes to comfort me and says ‘this is not like you’ and to find out what’s going on. I fleetingly wonder ‘what is like me, when I’m here?’ I feel bad because I know the team have had someone die today and one of the head nurses has had to race off and manage that. My tears over impacting my day with my hubby seem trivial in comparison and yet not, nothing is trivial in this Cancer journey. It’s all bearable for me most of the time, yet it is all sh*t too. I cry some more.
Nurse L comes to my rescue. She looked after me all last year and I missed her when she left to do a stint in private practice. She asks what is going on, I tell her, show her my empty box of Dex and say I just need my day 16 dose because I had to take it last night after not receiving the steroids yesterday. I don’t say which Nurse forgot to give me the steroid. Nurses are human. We all make mistakes. She is usually so so good so must have had an ‘off day’. AND, it was my mistake too. It’s not really fair to hand all responsibility and agency of my care over to a Nurse. After all, I bang on about being the agent in your own health and treatment for as long as you possibly can. Nurse L goes and gets the Dex dose immediately and finally I get to leave.
Thank you M and L. You saved my day. I know my Clinician plans to talk to the nurses about how the steroid was missed but I don’t worry about that now. I know mistakes happen yet between us, the Nurses and I are usually so good at going through a checklist each time. It’s a shame it went wrong.
On this day of all days.
Psychology Tips – Working with your and others’ mistakes

Admitting mistakes can be hard. Research shows there are links between our beliefs about whether we can change our behaviour or whether our personality is fixed and if mistakes and admitting mistakes are perceived threats.1 Cognitive Scientist, Art Markman summarised the research results2 and explains when you believe that your behaviour can change, you are more likely to be willing to admit responsibility. You recognise that by admitting what you have done wrong, you can work to make it better, to grow and so you are not threatened or are less threatened by admitting mistakes.
People who do not believe that they can change, can be stressed by admitting their mistakes, because they believe that those mistakes say something fundamental about who they are as a person. Understanding that people see their own mistakes as a threat, and have different beliefs about their own and possibly others’ ability to change, can help us to remember to avoid showing unhelpful frustration and anger when managing mistakes. We can all change our behaviour. We can all learn from our mistakes. We can all repair and improve relationships. It can take some people longer than others, to recognise that change and growth is possible, especially when their starting point is one of: I and others have fixed personalities and mistakes are flaws.
It’s easy to get frustrated with others’ mistakes when we feel something is unfair (it can be completely justified) but does it help the situation to show the frustration? A compassionate response will get you more powerful results and responding with anger and frustration negatively impacts loyalty3,4. In my case, I want the Nurses to like treating me. I want them to feel we are on the same team, to feel loyal, committed. Showing my frustration and upset was normal, human, yet unlikely to have been the optimal way to have managed the situation. Remembering that frustration, anger and stress raise heart rates, make it harder to think, mean that when recognising frustration, a good first step is to pause, be mindful, and then choose a more powerful response. One of clear communication, compassion, kindness, empathy, forgiveness. This is more likely to invoke compassion, kindness and loyalty in return.
Recognise too that anger, frustration and upset at mistakes of yours and others are often underpinned and exacerbated by worry and a catastrophising thinking style. I was worrying that my need to go to hospital on Hubby’s birthday day would ruin our day. Ruin his day. Eventually I managed to realise an unhelpful worry and thinking style was probably in play and ask myself, was my hospital visit really the worst thing in the world? Were my thoughts true, would our day really be ruined? How much time in our day did it take up really? Was it more likely that hubby was happy to help and had enjoyed his rare time alone, in a café, doing things he wanted to do, without having to be at work, while I was at hospital? Regaining perspective enabled me to let my frustration and upset go. An hour later I noticed I was laughing at something Hubby said and our day was going well. Yes, it meant we came home earlier than expected because I was really tired yet we relaxed together and the evening was a good one. I could easily have been very tired anyway. It’s not unusual for the day after Chemo.

References:
1 Who accepts responsibility for their transgressions? Schumann, K and Dweck, CS. Who accepts responsibility for their transgressions? Pers Soc Psychol Bull. 2014 Dec;40(12):1598-610. doi: 10.1177/0146167214552789
2 Markman, A. (2014) What makes some of us own our mistakes and not others?
3 Sara B. Algoe & Jonathan Haidt (2009) Witnessing excellence in action: the ‘other-praising’ emotions of elevation, gratitude, and admiration, The Journal of Positive Psychology, 4:2, 105-127
4 See Adam Grant, Psychologist and author of Give and take: A revolutionary approach to success. See also work by Emma Seppala, Center for Compassion and Altruism Research and Education.
Acknowledgements:
Shadow and Dex pictures by Me
Dog Photo by Matthew Henry on Unsplash
Shattered plate Photo by chuttersnap on Unsplash
Failed it Photo by Estée Janssens on Unsplash
© 2018 Janine Hayward www.psychingoutcancer.com. All rights reserved.
Posted in Chemotherapy for Myeloma, Myeloma Treatment, Psychology for Cancer, Symptoms and Side Effects Tagged with: Cancer, Carfilzomib, Compassion, Consequences, Dexamethazone, Frustration, Mindfulness, Mistake, Mistakes, Myeloma, Nausea, Psychology, Sick, Steroids, Sweats, Tears, Worry

April 9th, 2018 by Janine
Ahoy there…you may think I’ve been on some desert island and that accounts for my lack of communication. You’d be right. I’ve been in a world full of ‘I should blog’ and ‘I am blogging, it’s just that it’s in my head or on a random note, emailed to myself.’ That’s the funny thing about blogs…they’re there all the time yet not always out there….
I don’t know why I’ve put off getting my thoughts and stories out and about. I suspect it’s because I’d like to provide a great psychological tip each time I blog. Sometimes I can’t think of something I haven’t already said or I get tangled up in ’getting it right’. Then I end up not doing anything.
Paralysed. By what? Thinking something may not be good enough? Yet that’s not what this blog is about, at all. It is already enough. I blog when I can and when I do. I blog what I can. No more. No less. It’s helpful to me and hopefully, to one or more of you. It feels creative, a release.
It is what it is. I love that saying. It is so black and white yet YELLS acceptance. Can you visualise that? A phrase exuding and yelling acceptance. I love metaphors. I think I’ll ask my friend Sapphire if she might have a go at sketching this one, if she has time. She either will or won’t: both are fine.
Health status
I am doing fine. My mantra from the meditation I enjoy: I am doing fine. I am in my fourth month of the 18-month maintenance cycle of treatment. My results are no better, no worse. I get tired. My feet tingle sometimes painfully with neuropathy. I ache. Sometimes I have trouble concentrating, making decisions or being articulate. Often, I am the opposite. Out and about. On the go. Functioning well. Being me. Alive and living.
Eulogy
I said a very solemn eulogy last week. To my umbrella. My favourite umbrella that has been in the family for 13 years. 13 years! Do you know how unheard of, this is? It hasn’t been left on the bus or on a tube or in a café or lent to someone without ever being returned. It was a miracle of survivorship. It outlived all expectations. Especially with my record for losing things.
I loved that umbrella. It was a deep British green with a Jaguar car logo on it. A strong powerful leaping Jaguar. I love cats and especially big cats like panthers and jaguars (I even follow Jacksonville Jags NFL team since seeing them at Wembley a few years ago) and I have always liked the shape of Jaguar sports cars. This umbrella was perfect for me. It was small, light and a marvel of efficacy. Even the spring mechanism worked well every time.
I was so sad to see it go and I am yet to replace it. Living in England, particularly in Spring does not allow long before full commitment to another umbrella is required. It is of course, raining heavily again today. I wonder, will I channel my wonderful big cat umbrella and outlive expectations?
Who knew an umbrella could have friendship qualities? Always there. Reliable. Helpful. Comforting. Safe. I’ve been known to buy crystals, carry stones in my pocket at times. I wonder what other ‘things’ help others out there with Chronic Illness, Pain or Cancer.
Movie madness
I was sitting in the cinema recently and the lady next to me sneezed. Over and over again. When I’d sat down, I had noticed she had a blanket over her knees and thought nothing of it. After her first sneeze, a thought exploded into my head…oh sh*t, does she have flu? I don’t have a mask. Bugger, my immune system can’t get away from this one. Panic stations. Find a tissue, FAST. Cover my nose and mouth quickly.
I turned my back to her, snuggled into Hubby. I felt sad that a visit to the movies wasn’t straightforward anymore. I tried to focus on the film again. Then I started thinking, What was that like for her, for me to turn my back? Did she care? What did she think? Did she notice at all? If she did notice, was she making incorrect assumptions about why I moved? I hoped she didn’t think I didn’t like her, or feel rejected. All while these thoughts invaded my movie time, I prayed she didn’t sneeze again. She didn’t. She coughed, loudly. I felt angry. How dare she bring her bugs to the cinema. Get real Janino, everyone sneezes and coughs. Sh*t, sh*t and triple sh*t. I buried my head in Hubby’s jumper.
I started debating whether there was any point in turning away, covering my face with the folded tissue, trying to prevent bugs access to me and my vulnerable body? The little blighters get through anyway if they are going to…after all, most bugs are small enough to pierce a basic mask. That’s why I wear two masks whenever I’m on a plane. Picking up bugs, its unavoidable at the end of the day, isn’t it? Getting sick is probably unavoidable too. All I can do right now is keep giving my body the best chance of fighting off infection by eating well, being kind to myself, doing what I know to do to support my body. Accepting I’ll pick up bugs sometimes and focussing on the film is probably more helpful than getting angry and worrying about preventing any imminent attack.
We are under attack, by BREAD!

Did you know that there appears to be a big, big problem with much of the wheat we eat around the world – it is TOXIC! This is crazy, right? Glyphosate (in Roundup !!!) is used by conventional farmers, who spray it on their fields between plantings to reduce weed populations and for drying out grain and bean crops so the yield is higher. Did that sink in? A toxic weed killer is sprayed on much of the wheat that ends up in the bread we eat! What’s more, it has been sprayed on our bread FOR YEARS: bread that most of us have had in some form or another, EVERY day.
I’m so shocked! And angry!! The Netherlands have banned it. France are changing their legislation about it. The UK soil association is trying to get the UK government to do something about it. While the whole debate is becoming highly politicised there is evidence for the toxic cumulative effects on people’s health!!! Check out the articles below.
Frankly, I don’t eat a lot of non-gluten free bread these days anyway but I’m certainly going to try and go for organic only now too. I dont fancy consuming ANYMORE Glyphosate or Roundup! It is so damn hard to avoid toxins in this world! Or to know who / how to trust food producers. It will be so expensive if, to keep ourselves well or prevent disease, we return to buying EVERY food item at a speciality, boutique, or independent provider. Most of us simply can’t afford to do that, or it is impractical, even when we are able to work full time and whether we have cancer or not.
We live in wonderful times. We live in scary times.
I miss my brolly.
Check out these articles
The Scientist – How Toxic is the World’s Most Popular Herbicide Roundup?
https://www.soilassociation.org/our-campaigns/not-in-our-bread/
https://www.sourdough.co.uk/glyphosate-in-bread/
Acknowledgements:
Photo of the new version of my old brolly by http://davitcareditions.blogspot.co.uk/2010/11/jaguar-merchandise.html
Photo of sliced toast by Manki Kim on Unsplash
© 2018 Janine Hayward www.psychingoutcancer.com. All rights reserved.
Posted in Nutrition for Cancer, Psychology for Cancer, Symptoms and Side Effects Tagged with: Bread, Cancer, Cat, Gluten, Jaguar, Myeloma, Nutrition, Psychology, Toxins, Umbrella, Wheat

February 22nd, 2018 by Janine
Dr L turned to his colleague and said, ‘for someone with Myeloma, Janine’s immune system is a Schwarzenegger’. Hey Arnie, you are now a metaphor for my health status. Who’d have thought?! It sounds so positive and I am very grateful that my precious physical self is coping so well with the toxicity of Chemo. I notice too that I get a little hung up on the ‘for someone with Myeloma’ phrase though more about that in the next post. Now, I want to talk about my relationship with my body. It has become a bit confused.

Can I share a secret? I liked it when cancer, chemo and a diet change caused me to lose weight. I like being closer to 60kg than 70kg. I like how slim and less pear shaped my legs look. I like being size 10 and for a few weeks, size 8. All my life, I have valued being slim, strived for it. I’m not obsessive. I don’t over exercise or starve myself or think about it constantly. Even when I put on two stone from IVF treatment: I hated it but didn’t panic. The weight had context. Once we stopped IVF treatments, I lost a stone quickly and then worked on chipping away at the rest. I like cake. I binge occasionally (or did before this new eating regime). Who doesn’t when there is a pack of dark chocolate hob nobs in the house and the hormones are taking over? I would say I’m weight and health conscious with no extremes.

I’ve never liked my arms: they’re too big. Well, apart from the time I sanded every spindle on a stair case by hand: my arms were toned, like Madonna’s or Geri Halliwell’s. I thought my arms looked great after that. It didn’t last long. Finding tops and elegant shirts to fit my arms has always been a hassle. The welcomed side effect from cancer, chemo and clean eating has been the slightly thinner arms and shirts fitting, for once. I don’t really want to give that up yet…
I find myself struggling. I’m in a tussle inside my head. Too much weight and muscle loss is not healthy, not helpful and goes against Dr L’s advice. He explained that he had noticed that people with Myeloma who keep up with the gym and have some muscle reserve seem to manage the chemo better. I do want to live as long and as well as I can. Yet I find myself loving my new size. I bought a pair of boyfriend jeans a few months into treatment, laughing with a wave of pleasure when I discovered I could fit into a size 10 only to find they slipped off a month later and I’d lost even more weight. Now what do I wear? Nothing in my wardrobe fits!!
At that point, 61kg, it did get a bit worrying. My face was looking drawn. My rib cage and spinal vertebrae were a too visible. I promised Dr L that I wouldn’t let my weight fall further. I expanded my food repertoire slightly (good quality bacon, goats cheese, sourdough toast occasionally) and started the weight training.

Back at the gym, I felt good and waves of relief from feeling stronger. I’d become so weak. I was asking hubby to open jars and water bottles for me and lift anything. This does not fit with my independent and equality philosophy. Yet, I dislike how quickly my leg and arm muscles grow. When my weight started to rise slowly I would find it hard to like what I saw in the mirror. I know it may seem silly in others’ minds. Intellectually, I know I look ‘normal’, ‘healthy’ and would still look heathy even if I did put on weight (I’m fortunate to be tall). Except, somehow it feels like a tug of war in my brain – Janine, don’t put on more bulk, you look good as you are (now size 10-12) versus Janine, you need more muscle and strength to manage Chemo effectively, get yourself to the gym.
For more years than I care to think about, I have gone to buy clothes and come back disillusioned when I have needed that elusive size 13 or 15. It seems crazy to have the same problem at a lower size (now 9 or 11) and with the added complication of my size constantly changing. I can’t afford and wouldn’t want to invest in new sets of clothing every few months yet as my weight goes up and down on chemo, what can I do? Frustrating. I hate being uncomfortable in clothes. I really dislike ill-fitting clothes that don’t help me feel good and enhance how I look in the world. Too loose is as bad as too tight!

Even more annoying, last summer, before diagnosis, I bought some new clothes after ‘making do’ for a few years. Now they are sitting in the wardrobe, barely used as they are far too big. I am in the maintenance phase of treatment, with 3 days rather than six days a month of Chemo and my weight is climbing and fast. I’m 67kg today. Maybe I’ll need those ‘larger’ clothes again in a couple of months. Except, I don’t really want to get any bigger or go back to the size of those clothes again. The 6 days of steroids each month may have something to say about that.
67kg. Nothing to worry about. Yet, I don’t feel good about it. I am beginning to worry that a steroid induced, sharp trajectory up of weight, will set in and hang around for the duration of treatment. There are 16 months to go! That’s a lot of weight gain. That makes me feel sick.
It is also motivating. I’m back on the high veg and protein regime. A few bits of non-clean eating crept in as I celebrated getting through the first 48 (see previous blog) and 9 months of treatment. Then I let the goodies stay, it was Christmas after all. Then I felt sorry for myself with the arrival of two viruses back to back. January came and went, and it’s always the toughest month in UK for me. It’s so often grey, cold, hibernation inducing and all I want to do is eat comfort food!
Oh well, not having the clothes I would like, in the bigger scheme of things, is insignificant really. If I hover around the 65kg mark and I am made of tiny Arnie style muscles, that will be good enough. Viruses and January blues are gone. The revolution is here. February has arrived.
I’m back on track with preventing my body from being a perfect host for cancer. I celebrate a new food focus: FISH. It is easy to do: I am languishing on the beautiful beaches of ANTIGUA for a much-needed holiday. Fresh snapper, mahi and octopus are on the menu. The company is great (hubby and besties), the sun is high, the sea is warm and the forecast is rosy. No time for weight tussles now: The bikini is out and about!
Acknowledgements:
Antigua seascape: Photo by me
Legs and kettle bell: Photo by Maria Fernanda Gonzalez on Unsplash
Clothes hangers: Photo by Christian Fregnan on Unsplash
Shirt and Jeans: Photo by Lyndsey Marie on Unsplash
Muscles: Photo by Alex Boyd on Unsplash
© 2017 Janine Hayward www.psychingoutcancer.com. All rights reserved.
Posted in Chemotherapy for Myeloma, Finance and Cost, Psychology for Cancer Tagged with: Cancer, Chemotherapy, clothes, muscles, Myeloma, weight
February 6th, 2018 by Janine
A year ago, test results confirmed the specialist suspicions; I have terminal cancer, Multiple Myeloma. There is no cure. A year ago. Already. The last year has flown by. Three 2017 dates are now seared into my mind; January 30th, February 10th and my 48th Birthday.
A whirlwind of the new; hospital visits, medical terms and interventions, a community of haematologists, nurses, and Macmillan, a new language of cancer, psychology for self, learning, crying, toughing it out. Some days I said everything was fine, It’s OK that a hash was made of my cannula or I was waiting over three hours, again. Other days, I said ouch or OMG or Sh*t, that hurt, get me someone else please, you have not found a vein, this drip is not working, you don’t seem to be following protocol. I found and used my voice.
Every day I have appreciated the NHS, the team, the help, the efficacy and efficiency of Nurse M, A, and L and others M, J and J; their smiles, their hellos, the added lengths they have gone to and extras they have sent my way, a mask when I’ve needed it, a blanket, a ‘let me know if you need anything’, to ensure I felt kindness, cared for, human, me, Janine.
I’ve had a year of being on the other side of the badge. It’s not been me with the NHS credentials around my neck; they have had them. I walk the hospital halls that are so familiar but I’m not visiting a client, attending a seminar or meeting colleagues. Instead, the appointment is for me, the thick brown file of clinical notes are about me and the graphs and charts on the screen show my body, me, mine.
A year ago. Wow. I still find it hard to fathom. Things are normal but not normal. We get up in the morning. I go to hospital. Hubby goes to work. I rest. I tinker on projects. We go to the gym. We pay bills. Make dinner. Eat it. Watch too much Prime, too much Netflix (Vikings and The Crown, great, aren’t they?!). Life goes on. Yet it is all different, and the same.
I keep saying it ‘a year ago’ because it sounds so strange. It feels like I’ve been managing this for a few months, not a whole year. Last year on my birthday, I was getting second opinions. This year, on my birthday, I will be bunking off one week of Chemo to fly to sun, sand and sea. Thank goodness for that. Can’t wait.
Stress and Urgency
I’ve packed in quality moments in planned more. I’ve had a year of panicking that I may not get the opportunity to see that person again or go to that place. A year of thinking, ‘don’t delay’, get on with, the before I die, I want to, list.
Deep breath. The year has passed. My urge to live life urgently is still there yet the urgency has evolved, is more measured, less reactive, calmer, I think. I hope. I discovered my need to move to Italy (a lifelong dream) is not so intense and possibly not what I want at all. Instead, to be able to travel there frequently and for longer periods of time may suffice and be less stressful (more affordable, more flexible, without the bureaucracy and difficulties of moving to a new country). Or am I compromising too much? Time, I’ve decided to give it a little more time. The right thing will become clear. I’m lucky, I’ll be here tomorrow.
Stress in life is normal, even needed. Now, as my own therapist proposed, the best question is, which stress is worth it? I do still worry (in line with what we currently know about the likely progression of Myeloma) that the next two years will be my best, my healthiest, my most mobile. I do hope to plan and pack in lots of lovely adventures with great friends in 2019 and 2020; ski, sail, bike, travel. Maybe even have a big party or escapade when this 18-month round of Chemo is over. Although, I’m not wishing my months away just yet.
It’s also OK to not go crazy; spend everything I have on adventures or abandon everything I had already planned and put time in to. It’s ok to think I’ll be around for a long time (15 years would beat the odds) to invest in our home, our future, and believe, I will have time to enjoy the benefits of the investment.
Feelings
I feel a bit weird yet I don’t really know how I feel, one year on. A bit unnerved, numb, maybe? Strangely alive at other times. I haven’t really worked it out yet. I wonder if I’ll ever know? What will show up if I let it? Over the next few weeks? Over this entire journey? The new, yet strangely same life of mine, of ours, that now includes and accepts cancer yet is a life, lives, that refuse to be made invisible, small and weak.
A year ago. What happened to you over the last year? Did you grow? Flex? Build resilience? Laugh, love, cry and learn? I hope so (more laughs than cries with luck).
I have.
© 2017 Janine Hayward www.psychingoutcancer.com. All rights reserved.
Posted in Diagnosis, Psychology for Cancer Tagged with: a year ago, Blood Cancer, Bone Cancer, Cancer, Crises and Stress, Myeloma
December 6th, 2017 by Janine
What a year! I turned 48, I was diagnosed with cancer and I’ve completed 48 chemo sessions. I love the number 48; it seems so symmetrical to me (I love a bit of symmetry). Now ‘48’ has a WHOLE new world of associations!
Warning…I have happy news, and, I’m going to talk about toilet rituals.
First, the rituals.
This may seem very strange to those of you who have always been super careful about hygiene when using public loos. In my defence, I have rarely worried about these things because my childhood in New Zealand was filled with non-traditional toilet arrangements. When you are fortunate enough to spend all day at the beach or walking in the bush or driving long stretches of deserted road or camping in remote sites you tend to get over yourself quite quickly about going to the loo wherever and however.
Doing your business quickly behind a tree, rock, or in a smelly long drop with minimal paper or alternatively leaves or seaweed, is not that unusual. Worrying about being seen was always a bit more bothersome than worrying about bugs, microbes or possible infections! The upshot is; I have never worried about using public loos, ‘catching anything’ or having to use disinfectant. I just focussed on washing my hands well.

Now that my immune system is compromised it’s another story completely….though maybe I’m being a bit anal? (pun intended)
In the Chemo Day Unit, patients are asked to ‘wipe the loo’ with anti-bacterial wipes before and after use. I recently discovered I had developed a wee ritual…Take a wipe, clean toilet seat, fold dirty side in, use clean side to wipe toilet handle, tap, hand wash dispenser, door lock, door handle. Dispose of wipe in bin. Use loo. Wash and dry hands properly – you know the 8-10 step process (depending on the poster). Take new wipe and clean toilet. Goodness knows what bugs I could pick up if I didn’t do this; don’t tell me!
Anyway, this is a new ritual in my life and once again one that seems to consume a little more of my available time and life though hopefully is worth it. It seems so, so far, as I have yet to pick up any major nasties despite lower immunity and chemotherapy for 9 months now. This ritual has now made its way out of the hospital and into public conveniences. AM I being anal? I’ll let you be the judge!


My News
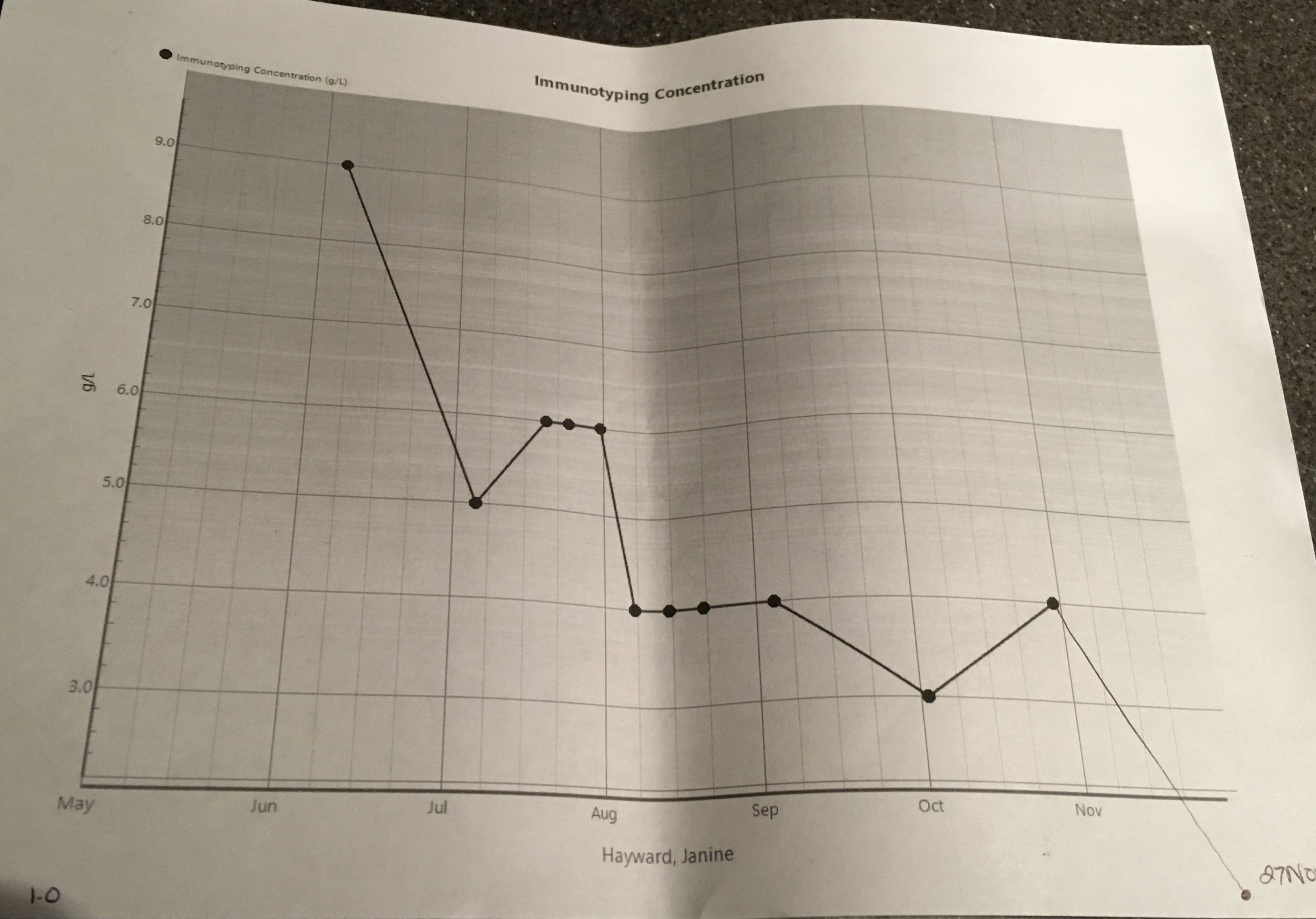
…is happy, positive and hope-FULL…I’m very grateful for it and its effect; a reaffirmation of my faith in my medical team, the drugs and my health and life choices. The Myeloma presence in my body has decreased further in the last few months… It’s down to 1 g/l (42 g/l at its peak) and a may be yet to plateau. Yee ha! Not only that, the serum kappa light chain results are 1.75 mg/l, backing up this great news and described as ‘excellent’ by Dr L. On top of that my liver is doing well. My Hb (Haemoglobin, the protein found in the red blood cells that carries oxygen around) level is back up to 121 g/l so I no longer need to consider taking EPO (yes, the cheaty cyclists’ drug of choice! I’m a tad disappointed. I had wanted to experience how energised I’d feel!) While 121 g/l is lower than the desired normal levels (125 g/l plus) it is great for someone with Myeloma. My kidneys are also doing OK for someone with Myeloma, my Creatinine is 69 umol/L and normal level for women is approx. 45 -90 umol/L (I think; there seems to be some debate!). Lots of good, great news, here. Dr L delivered these details and then reminded me to keep drinking 2-3 litres of water today for kidney care. I imagined my kidneys; bloated, water-logged, bean-shaped balloons, wrapped up in clouds of cotton wool, floating about, relaxed and without a worry in the world.


I’ve had yet another bone marrow biopsy and pet scan (what effect does three doses of radioactive sugar chasing gunk in a year have on one’s body? I guess I’ll find out!). I have an ear numbing full body MRI coming up in a fortnight.
Let’s hope they show (or don’t show lesions at all) that lesions are further dissolved and there are no new uninvited guests!!
What a year.
48.
One number I’ll never forget.
Acknowledgements
Images: Me (graphs va KCH), Long Drop – Sarang (public domain use permission granted)
© 2017 Janine Hayward www.psychingoutcancer.com. All rights reserved.
Posted in Chemotherapy for Myeloma, Myeloma Treatment, Results Tagged with: Bone Marrow Biopsy, Chemotherapy, Myeloma, Results, Tests, Treatment

October 31st, 2017 by Janine
OK Mr Tumour or more accurately Messrs Tumours. Listen up. Yep, all four of you. You know who you are. You are hanging around unwanted and uninvited. Where do you get off thinking its ok to be dossing about in my body? You’re a greedy bunch, aren’t you? Not contented with one spot, you hunker down in two places in my spine, my shoulder and my sternum. You threaten me with paralysis as you near my spinal cord and grow dark and big. What arrogance! Well, I have some words for you.
I have mindfulness and meditation and you are not going to like them. In fact, I already know you haven’t seen them coming. They have roughed you up a bit with their calm, kind, ease. Aww. Tough. If you can show up unannounced, I sure as hell can unleash mindfulness and meditation on you.
Your resistance is futile. You are already weaker. You can keep trying to hide out, munch on sugars (if I give you any) and try to take over the joint…but I know where you are. Your luck has run out. The Chemo is working. My new diet is working. My NHS medical team is great. I am doing fine. My mindfulness and meditation practice, reminds me this is so. Mindfulness and meditation practice, whether 5 minutes or 35 minutes; it’s getting to you, Mr Tumour (yes you, the large one in my lower spine). I’m talking to you.
YOU are DISSOLVING.
One at a time. Worst, darkest, nastiest first. You are dissolving. I know because I have seen you. My MRI showed me. You are thinner, lighter, dissolving, dying. Don’t feel bad. You are no match for kindness, curiosity, breath, acceptance, listening, powerful visualisation, practice of belief. Belief that my decisions about my treatment have been the right ones for me, that my medical team is the right one for me, the Chemo is the right Chemo for me and that I am doing fine.
My favourite guided meditation reminds me of this.
NOW you are DISSOLVING.
Meditation helps me visualise an all-powerful, protective, transformative, warm, healing light. It wraps up all four of you, Mr Tumour, you and your buddies, letting you know you are not needed. The light heals my body, generates new healthy cells, rids me of you. This same meditation helps me draw energy, power and peace from the Universe, imagine, believe and trust I am in safe hands, doing the best I can do. It is working. You are not running this show or in charge of this gig. I am; with the help and support of mindfulness and meditation.
Mindfulness for sleep. Mindfulness for Cancer. Mindfulness. It helps me to stop. To be. To breathe. To observe. Mindfulness, paying attention, moment to moment, in a kind, curious, non-judgemental way. Not like you, Tumours. You are random, cruel, unnecessary. Yet, thanks to Mindfulness, I accept you. I accept that you are here. I watch you, learn from you, ignore you and listen to you. I accept you have muscled your way in, demanded to be seen, to be heard. With Mindfulness, you don’t get to invade my every moment or even most moments. You don’t get to hurt my sense of who I am. You don’t get to take over. You get to be. Until, you are no longer being.
Listen up Mr Tumour. You are superfluous to requirements. While I accept you are there, I’m just letting you know you can go and take your friends with you. I know you are likely to return in the future; I’m a realist. Right now, you are not needed and not wanted. By the time, you want to make a comeback, I will be stronger than I am now, even more practiced in mindfulness and meditation, and healthier with years of a great low sugar diet behind me. I will have more chemo options and more effective medical solutions at my disposal. I will know more about you, your characteristics and the environment you need to thrive. I won’t provide it. You’ll have to find somewhere else to go or better yet not bother at all. I am ready now. I will be ready in the future.
I might have dark days and dark weeks through this journey Mr Tumour but that is nothing on how uncomfortable I am making things for you. I am not going to fight you. I’m not in a battle. I simply will not be providing the terrain that you want. I see you. You are dissolving. Soon I won’t see you. You are getter weaker. Myeloma may remain but you Mr Tumour are no match for my healing light. You do not have to stick around. Mindfulness and meditation, they’ll remind me why you came and what you can teach me. I won’t forget you. I don’t however, need you. I will watch you dissolve. You can leave now. Thank you.
Three of my favourites;
Meditation
Survive Thrive and “Dawning of the Day” by Aine Minogue
https://youtu.be/MNaqEKtc4Uk?list=PL2a9c2CFCJdlYehE9jochHrjWFMq4AHiu
Mindfulness
https://www.headspace.com
http://franticworld.com/resources/free-meditations-from-mindfulness-for-health/
© 2017 Janine Hayward www.psychingoutcancer.com. All rights reserved.
Posted in Chemotherapy for Myeloma, Psychology for Cancer Tagged with: Cancer, Dissolve, meditation, Mindfulness, Myeloma, Nutrition, spine, Tumour
August 22nd, 2017 by Janine

Hooked up
My blood spurts everywhere like a regular Fright Night or Halloween movie. The nurse is trying to put a cannula into each arm, a bloody big cannula, much bigger than my normal (ha ha) Chemo cannula. The nurse is new to this treatment and seriously nervous. Great. I’m not in the mood today. The mood. The mood where I am happy to be part of someone else’s learning curve. I’m just not. Now she’s made a mistake and there is blood everywhere. My blood. My very, very, precious blood.
Another nurse pounces with a clamp and gets everything back under control. For now. Except, I feel sticky. My leggings and legs are spattered with blood. The pillows and bed coverings are no longer pristine white. Stressed, I blurt out, ‘I don’t want to be anyone’s experiment’. The nervous nurse (NN, my nickname for her) looks horrified. She reassures me that I am nobody’s experiment. Her body language and voice sound like she is trying to convince herself that everything is OK. I think ‘I can’t afford to lose any more blood; get me someone who has done this A LOT’. But I don’t say this out loud. I hope it, instead. I calm down a bit and give NN, a smile of, ‘it’s ok’. It’s not OK but I figure I need her to be calm. Everyone makes mistakes. In the grand scheme of Myeloma treatment, this wasn’t a bad one (so long as I don’t end up needing that runaway blood).
I am in the Apheresis unit, finally all wired up (ready for ‘take off’?) to a clever centrifuge machine (very CSI) labelled 3OJO (MOJO with a 3? A machine with 3 times the MOJO?). Anyway, this machine specialises in taking blood out of one arm (Vampire-esq), separating out plasma and stem cells and then giving what remains of my blood, back to me, through the other arm (Angel-like). Genius! my niece would say.
I try to relax. The machine’s sound reminds hubby of ‘‘beedie beedie’ so we nickname it, Twiki, and completely ignore the OJO’s in the end. Do you remember the TV show called Buck Rodgers? Twiki is a silver robot (cute but with unfortunate haircut) known in the show for saying ‘beedie beedie’ to everything. Very effective. I’ll think I’ll use it.

Twiki with a lot of mojo (Stem Cell Collection machine)

All the fancy stuff Twiki monitors
I’m quite intrigued by my blood and its component parts…hanging in a bag next to me is the plasma, a funny yellow colour and next to it, slowly, salmon pink (apparently, that’s a good colour) stem cells appear. Also on the line in bags are saline (isn’t it always?) and an anti-coagulant. My lips begin to tingle strangely and I feel a bit faint. I let the nurses know. They have warned me this can happen. My calcium level is ramped up and I’m lowered down a bit in the bed. A song pops in to my head…Blood, Blood, Glorious Blood…There’s nothing quite like it…My Glorious Blood.
Boredom kicks in for hubby soon after arrival, I’m not very talkative today. I can’t sleep because to help collection along I am required to pump the stress ball, all day, only taking breaks for a few minutes every 10-15 minutes. Hubby checks out all the bells, whistles and knobs on Twiki and marginally resists touching them (knobs after all) and is now entertaining himself by dancing on the spot. I’m trying to work out which music he’s listening to because he occasionally is singing out loud, unintentionally I think, and boy his lyrics are dubious! The nurses and I catch a look and laugh. Glad he’s got a day job! Though I’ve secretly always loved his dance moves. I still can’t work out which songs he is listening too. Turns out he’s immersed himself in 70s and 80s and he’s running through Hall and Oates hits (would never have guessed). We share headphones and have a laugh with the past. Today is turning into a retro day.
I arrived at 8.30am and it’s now 5pm and I too, am very bored; so ready to be out of here. I’m waiting for lab results to come back and say they’ve taken enough stem cells. For the last four days, I’ve had G-CSF injections that stimulate the stem cells to move out of my bone marrow and into my blood so Twiki can collect them. This is preferential to the other option of having them collected directly from the marrow (painful, long, more chance of complications, I suspect).
The injections have some seriously weird side effects; they cause pain from inside my bones (ironically similarly to the way Myeloma does…there are so many ironies with this overall treatment process, seemingly making things worse in order to make things better!). At random points, shots of pain would pulse from my rib cage or my pelvis, take my breath away and stop me in my tracks. It would usually be gone within 5-10 minutes and then be back again 10 minutes later or half an hour later or whenever it decided!
Lab results this morning told me the injections had ‘done their thang’ and the detectable level of stem cells in my blood (CD34+ test) was well over the count required to go ahead with Twiki’s collection manoeuvres. Thank goodness. The collection target is 7 million stem cells per kilogram of body weight and I hope it can be done in one hit, today. The results come back and they are good but I still need to rock back up tomorrow (and take another injection). They have collected 5 million. A few more are needed. Hubby and I walk home slowly. I feel shattered.
I’m baaackk! The next morning is a funny affair, no more escaping blood and instead a new approach. Yesterday’s senior nurse seemed to be cautious in approach, going slowly and setting things up so blood clotting was avoided. Today’s senior nurse explains she prefers to deal with problems when they arise and ‘we’re going to go for it’ and monitor everything carefully. Funny, I thought coming in two days in a row for the same treatment would ‘be the same’; a standardised process. I hadn’t factored in the human element and the nurses’ different strategies. Today’s target is 3 million stem cells per kg of body weight so info is plugged into Twiki and I lie back and ?? think of England? More like think ‘please please collect everything needed quickly’. It’s an all-day affair again. My potassium and calcium levels need propping up so I go home with extra meds to add to my ever-growing list.
The call comes through an hour later; they’ve collected another 5 million. Excellent that’s 10 million stem cells altogether. They’re sent off for cryopreservation (storage in liquid nitrogen at some crazy temperature, −196°C). I’m relieved. Maybe that’s enough for three transplants in the future. Maybe I’ll live longer thanks to these. If that’s the case then this last week has been a tiny investment; completely worthwhile.
Turns out from discussions with my clinician later that three transplants are not routinely given at the moment and there is no evidence supporting their benefit. Instead, the transplant team would usually spilt the 10 million stem cells gathered into two larger lots, for each of the two transplants. Supposedly there have been some benefits found for higher amounts of stem cells being used per transplant.
Oh well, you never know. By the time, I need the second one maybe they won’t need as many cells after all and I can eek out another transplant. Or my transplants will be so successful I won’t need a third one. Or it will be what it will be, completely in line with current evidence and practice. I’ll worry about that when it happens.
As part of the clinical trial I am on, I’ve been randomised to another four months of chemo (Carfilzomib, Cyclosphamide and Dexamethazone, half the Dex dose than in the previous four months) rather than an immediate transplant. I don’t need to worry about the transplant details right now unless something goes a bit wrong and the Myeloma comes back with a vengeance sooner rather than later (after all it is always going to come back). I crash for two days (the cat loves it) and feel really shattered for the week.

Post collection rest
The good news about my Myeloma is that its presence in my body after the first four months of Chemo has dropped; the IgG kappa paraprotein level is down to 6g/l after being as high as 42g/l. It’s not quite the 100% response rate I was hoping for but it is damn good. It is not usual for this rate to rise again for a year. I’ll have regular tests and jump on it if it decides to buck the trend.
I’m a bit low in mood and I think this is mainly due to low potassium and not knowing what the next phase of treatment is. Dealing with uncertainty is tough and coping well with it, ebbs and flows. That’s normal. I have talked about this in previous blog posts. I’m also nervous (my turn). I have a pet-ct scan coming up this week. Will the radioactive sugar stuff sent into my body find new lesions in my bone marrow, new weak spots or confirm that the treatment has worked brilliantly so far?
Maybe it is a good time to explore my relationship with illness and health. I can step out of project mode for a moment, round one of treatment has been accomplished. Now, is as good a time as any to face asking myself, in a more structured way, what it means to have incurable cancer, what it means to be ill. Which factors, which thoughts, beliefs, feelings and sensations are influencing my health behaviour, my coping…and not coping?
Psychology
One established psychological and behavioural model for explaining how we think about, respond to and manage threats to our health is Leventhal’s common sense model of self-regulation of health and illness1. Here are three of the concepts at the heart of the model.
- our perceptions of our illness directly influence our coping strategies, which in turn influence outcomes.
- our perceptions and resulting mental representations of illness and health threats have two parallel processes, a cognitive representation (our beliefs about; our identity, causes, consequences, timeline, coherent understanding and control/curability of our illness) and an emotional representation (our fear, distress, anger, worry, depression, guilt or other affective states). We use these mental representations to make sense of threats to our health.
- we actively engage in problem solving by testing coping strategies (aimed to manage fear from emotions, and danger from cognitions), and checking whether the coping strategies have worked, to help us reach goals (e.g. to overcome cancer, to survive as long as possible, to overcome anger and be the person we wish to present to the world/think ourselves to be despite illness or to be well enough to play with our children every day)
The model is one way of explaining how we go about reducing the tension that arises between holding on and letting go of important values and goals as we come under threat from ill health, disease processes and treatment impact and side effects. Figure1 below shows this in a bit more detail.
I thought I’d use this model to explore my thinking, beliefs, biases and assumptions about my current health. If you are managing pain, chronic illness, cancer or caring for someone who is ill, I hope you find it helpful to ask yourself similar questions. I encourage you to notice the thoughts that pop into your mind without judging them; they may surprise you. When I work with clients who are living with ill health using this model, they often discover something that they had no idea was influencing their sense of self, or making them feel worse or they discover a rule they had imposed on themselves, based on an unchallenged belief about what it means to be unwell or to be going to hospital or taking medication.
Where to start?
I start by asking myself;
what does ‘health’ and ‘being healthy’ mean to me?
what does being ‘ill’, ‘ill health’, ‘being sick’ mean to me?
Do these concepts mean different things when I think about myself versus when I think about others?
What does it mean to be diagnosed with cancer? With Myeloma? What does it mean about me that I have been diagnosed with cancer, with Myeloma? If it was my partner or a stranger with the diagnosis how would the meaning of having cancer/Myeloma be different?

Figure 1. Hagger and Orbell’s (2003) schematic representation of
Leventhal’s (1980) Common Sense Model of Illness (CSM).2
What do I ask next?
I explore a range of questions with myself about the mental representations I have about being unwell and under threat from cancer. While I work through each question and consider my answers, I also explore how my responses make me feel and what I will do to cope with the event and the feeling.
Stimuli
What am I experiencing?
What are my symptoms? (e.g. pain, fatigue, breathlessness)
What is telling me I’m unwell? (test results, pain, reduced mobility, hospital appointments)
What do I know about my illness?
Where is my information coming from? (external: medical team, support groups, google, other patients; and internal: physical and mental experiences)
What are my symptoms? (e.g. pain, fatigue, breathlessness)
What is telling me I’m unwell? (test results, pain, reduced mobility, hospital appointments, calls from medical team)
What do I think about where the information is coming from?
Cause
What do I think has caused my illness? Do I think any of it is my fault? Someone else’s fault? How has my illness come about? What do I think about the cause/s?
Consequences
What are the consequences for me, of my being diagnosed with cancer? From being unwell? What will I be able to do and not do? Will my life change? How will my life change? How will my relationships change?
What are the consequences for others of my being diagnosed with cancer? From being unwell? How will their life change?
Control /Curable
How much control do I have over what is happening to me? Over being sick? Over getting well?
How much do I think and believe my illness is; curable? able to be overcome? able to be managed well?
What do the consequences of the illness (e.g. likely outcomes, treatments, having to have chemo, a transplant, hospital visits and beyond) mean about who I am? what I am? My capabilities? My sense of being a woman? A daughter? A wife? A lover? An academic? A clinician? An exercise bunny? A coffee lover? Looking at all the aspects of my sense of self what does being ill, having cancer mean for each of those and who I am? No change? A change? For better? For worse?
Timeline
How long will I be ill? Will any changes and consequences be temporary? permanent? If my life changes will I be able to change it back once I am well or coping with the illness? Will it be the same as before?
Emotions
In addition to any coping strategies captured while gathering responses to the questions above…
How do I feel overall, right now, today?
How do I feel about being unwell? How do I feel about having cancer? How do I feel about each aspect above; the causes? The consequences? My sense of self? The controllability? Curability? How long I’ll be unwell? How do I feel about each of these? How do I feel about my thoughts and beliefs about each of these?
Coping strategies
In addition to any coping strategies captured while gathering responses to the questions above…
How will I cope? What am I trying? What makes me feel better? Feel worse?
What will I do? What will I avoid doing? Will I ask for help? From who and where will I ask for help? What will I practice thinking? Not thinking about? Where will I put my energy? What will I focus on? Avoid focussing on?
What emotions will I allow myself to express? Are there any that I am not happy to express? Why?
Appraisal of coping so far
What has worked well so far? What helped the coping strategy to work well? What hasn’t worked well? How did it not work well? What were the outcomes?
What do I want to change, try next, no longer try?
Working through these questions and using this type of model is challenging to do alone and isn’t something that is likely to be done and dusted in one sitting or even one day. It may take time to make the enquiry of yourself and find your answers. Notice the answers that pop into your thoughts, into your head. The answers may be scary sometimes, difficult to acknowledge or leave you feeling upset and distressed.
It is important to be kind to yourself during this enquiry. Its ok to take breaks. Its ok to feel distressed after noticing the answers. It’s a good idea to do something nice for yourself after working through these questions. These are difficult questions for anyone to look at, let alone anyone who is living with ill health or a life-threatening health concern.
Remember the aims of making the enquiry is to
- understand how we are making sense of our own health, ill health, diagnosis and health journey
- notice the factors influencing both our coping strategies and our appraisals of the outcomes from our chosen methods of coping.
- identify coping strategies that are likely to be most useful (complement our treatment and enhance our behaviour and management of illness, Myeloma) and drop the strategies that don’t work so well
Ultimately, by bringing our mental representations into our consciousness, our awareness, we may be able to pause and challenge some of them, more easily accept others, and create and foster new helpful health representations.
Many patients perceive they can stand extreme toxic Chemo therapy when they also hope and feel that it may result in a cure.3 There is no cure for Myeloma so how do Myeloma patients, how do I, stomach Chemotherapy? Do I stomach it because I hope it buys me time for living and time for a cure to be found, or buys me less pain, less discomfort, more quality of life? How am I managing fear control and danger control? What are my representations of illness? How vulnerable am I? How motivated am I to take self-protective steps? How easily accessible is my motivation? When is it easy, when is it difficult, for me to do the right things, to look after myself, adhere to medical advice, and adhere to the other complimentary advice I have chosen to follow?
Watch this space – I’ll post my answers over the next week or so to give you an idea of what this type of enquiry might look like…and then I’ll talk about what you might do with knowing your answers – how bringing the answers into your consciousness can help us to better manage the challenges that face us, illness based or otherwise.
Right now, I need a break so I only have one answer for you…
Beedie Beedie.
References
1 Leventhal, H., Meyer, D. and Nerenz, D. (1980). The common sense model of illness danger. In: Rachman, S. (Ed.), Medical psychology, Vol. 2. pp. 7–30. Pergamon, New York.
https://www.academia.edu/259452/The_Common_Sense_Representation_of_Illness_Danger
2 Hagger, M. S., & Orbell, S. (2003). A meta-analytic review of the common-sense model of illness representations. Psychology and health, 18(2), 141-184.
https://www.researchgate.net/publication/250571403_A_Meta-Analytic_Review_of_the_Common-Sense_Model_of_Illness_Representations
3 Cameron, L. D., & Leventhal, H. (Eds.). (2003). The self-regulation of health and illness behaviour. psychology press.
https://books.google.co.uk/books?hl=en&lr=&id=P3UoIuANmrIC&oi=fnd&pg=PR8&dq=The+self-regulation+of+health+and+illness+behaviour.+psychology+press.&ots=ARDdFKnVmY&sig=hU9R0fsNauKIs04RB3iezy-yAyA#v=onepage&q&f=false
Posted in Myeloma Treatment, Pain, Psychology for Cancer, Symptoms and Side Effects Tagged with: Apheresis, Cancer, Clinical Trial, Fatigue, Harvest, Myeloma, Para Protein, Psychology, Randomisation, Stem Cell Collection, Therapy, Transplant
July 19th, 2017 by Janine
I’m going to be sick. I’m running to the bathroom. I’m not going to make it. I’m scanning for basins and thinking use the kitchen if I can’t make it to the bathroom. At least make it to the tiles, it will be easier to clean up. I make it, this time. While I’m trying to keep my hair out of the toilet bowl and not notice how sore my knees are on the floor I start thinking; Where did this nausea come from? The last three months have been relatively easy; is this what Chemo is really like? Is this the nausea others talk about? Well they can have it back; it’s awful. And it’s not the worst thing.
I slowly make it back to the couch and lie down. I’m wondering if this last month of induction treatment is worse because I have responded so well to Chemotherapy over the last few months, now there is less cancer to vamoose; more good cells are copping it. I’m thinking about this when I notice my brain is getting hot. Not my head, not like a headache; my brain. In fact, its not just hot, it’s getting hotter by the second. My brain is on fire and I’m not sure I can cope. My eyes feel heavy…and hot. I can’t keep them open but I feel sick and am going to have to get up any second to go to the bathroom again. At this rate I’m going to need a couch near the bathroom or in it, not that it would fit. My brain hell fire is getting worse and my body is screaming at me to close my eyes, sleep, now!
I can’t, I have to go back to the bathroom. Ginger tea isn’t working this time. The anti-nausea pill isn’t working either. This chemo experience is different, and besides, I can’t keep anything down. So much for gaining weight or staying hydrated. A bit hard to do when I’m vomiting. I manage the journey to the bathroom, throw up and hang out for a while waiting for the next wave of nausea. I have a picture of my brain burning bright yellow and red with solar flare flames coming off the top of it, searing their way out of my skull. My brain feels like it is about to explode. It’s excruciating. Am I literally being fried with chemicals? I make it back to the couch and succumb gratefully to sleep.
From 4pm to 2am I’m in the bathroom or asleep. When I wake I feel trashed, tired but better. I eat two rice cakes and marmite (love it or hate it, it has its moments) and manage to take my meds. Relief. I feel slightly normal again. I watch TV for an hour and go upstairs to bed.
Sleep has been elusive over the last three to six months. I often wake every 1-2 hours. I am feeling a bit low and constantly tired despite the steroids. Unsurprising really when I’m not sleeping well. I talk to Dr L about pills and the nausea/brain fire. He takes control and agrees sleeping pills are a good idea and proposes a second anti-nausea drug. He doesn’t want me ‘putting up with’ anything. Relief again. I am finally going to get a good night’s sleep. Florence pops into my mind.
Music; Dog Days are Over, Florence and the Machine
For the first three months/rounds of Chemo I’d had no anti-nausea help and found using simple ginger tea worked. Now, I’m using two lots of anti nausea meds and ginger tea. The pfaffy thing; I need to remember to take the new meds 30-60 mins before food, three times a day. More stuff to think about when there are already so many pills and supplements to keep a handle on and information about upcoming treatment to process. Still, I’m highly motivated to prevent “brain on fire” and vomiting every five minutes – funny that.
The flag at Kings College Hospital is at half mast during my hospital visit, appropriately, for the victims of the horrendous attacks in London and Manchester. I feel strange too; grateful for not being in one of my favourite areas of London, an old stomping ground, at the time the attacker was there and yet also wondering how I would have reacted if it was me the person with a knife had come after. Does knowing you are dying sooner than expected change how you might react in crisis? Would I have run or taken more risks? Thrown things at the attackers, tried to fight back or help those that had been stabbed? Who knows? I can’t know. I’m grateful in many ways for not knowing and yet I’m curious about whether I would be different now.
The rest of month four passes without too many glitches and the best thing is getting some sleep – hurrah! I’m a bit depressed about how much strength I’ve lost though, and how old I feel when I can’t undo a jar lid or carry something I’d usually be able to carry. Weight training is now 20 reps of 1kg weights rather than three sets of 12 reps of a much higher weight. Fatigue is ever present.
This is not a novel new project anymore. The chemo, the eating regime, I’m over it. I want a break.
Editorial Support: Stephanie Kemp
© 2017 Janine Hayward www.psychingoutcancer.com. All rights reserved.
Posted in Chemotherapy for Myeloma, Myeloma Treatment, Symptoms and Side Effects Tagged with: Brain, Cancer, Fire, Myeloma, Nausea, Sick, Side effects
































